You finished the case! Now what?
As prosthodontists around the country are gearing up for the 7th annual National Prosthodontics Awareness Week (April 8-14, 2018), there will be a variety of public awareness campaigns to educate dental professionals and consumers as to what the specialty of prosthodontics is all about. This year I have chosen to dedicate time to raising awareness for the dental “after party”. What should we be doing for our restored patients, and what should they be doing at home to help improve the longevity of their dental investment?
A Review of Clinical Practice Guidelines
Although not a new publication, it was truly the first of its kind when the Clinical Practice Guidelines for Recall and Maintenance of Patients with Tooth-Borne and Implant-Borne Restorations1 was published in several dental journals in 2016. Many authors took part to help develop basic guidelines for the dental profession. Our clinical evidence for the majority of what we recommend has come from few randomized clinical trials and many times is just expert opinion. Preventive care, unfortunately, is not alone in this arena, but remains one of the biggest questions for us and our patients. Let’s review the highlights of the published guidelines.
Patient Recall
Recall or recare is one area that does not have complete consensus in terms of recommended time intervals for patients with fixed or removable tooth-borne or implant-borne restorations. An annual exam is typically recommended for several reasons, but what about bi-annual? One of the more powerful statements from the guidelines is that patients with complex dentistry need lifelong professional recall regimens that are individually tailored. As patients age and their restorations wear, more frequent recalls may be necessary. That might be every three to four months for professional maintenance, whether they are periodontally involved or not. Several studies have shown patients with removable or implant-borne prostheses are more likely to have complications that will affect the lifespan of their prostheses, if they are not maintained professionally. In other words, people that disappear from the dental world after having spent time and money on their mouths, are likely headed for more problems. It is important to decide on a recall schedule on a patient-by-patient basis, and to decide what is included in their recare appointments.
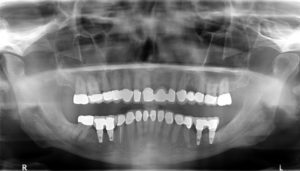
Fig. 1 Combined Tooth-Borne/Implant-Borne Restorations
Professional Maintenance
We have clinical evidence to support the benefits of professional maintenance for the dentally restored patient. As mentioned previously the time intervals will vary between patients, but the clinical guidelines recommend detailed examinations for both tooth-borne and implant-borne restorations, reinforcement of oral hygiene practices, and application of topical agents when deemed necessary. The use of topical fluoride and chlorhexidine continue to remain as two beneficial therapies to help prevent recurrent caries. There is also new evidence for the type of debridement for implant supported prostheses. It is preferred to have a compatible material for implants (titanium scalers), and new evidence suggests air polishing systems using glycine powder may be more effective and less harmful to our components. There is no consensus on fixed hybrid restorations and how often they should be removed. This is a decision that should be made on an individual basis. Perhaps the most helpful reason for having professional maintenance is to continue to reinforce to our patients what they can be doing at home to help their dental restorations go the distance.
At-home Maintenance
Last, but not least, is how we educate and equip our patients to perform at-home maintenance. We have evidence to support the use of highly fluoridated toothpastes on a regular basis (3-4 times weekly) for tooth-borne restorations. There are also recommendations for weekly chlorhexidine rinses for patients with both tooth-borne and implant-borne restorations. I will probably burst a few bubbles by saying there is very limited evidence to support the removal of removable prostheses at night, whether conventional or implant
supported. There is also limited evidence to support the fabrication and use of nighttime oral appliances for bruxism. Most “experts” have recommended this for heavily restored patients, but we lack sufficient evidence to say they need to be used for every patient. With that being said, what do we tell our patients? Once again, our recommendations should be on an individual basis, depending on the restorative category, and must include other variables like patient health, xerostomia, periodontal history, peri-implantitis history, and parafunctional activities. With patient education and awareness, we cannot necessarily guarantee our work, but we are attempting to provide the longest lasting restorations possible. The implementation of a recare system that is specific for our restored patients will likely turn out to be the best preventive dentistry we can provide.
I hope this edition of the Byte has been helpful. An online summary of the Clinical Practice Guidelines is available at https://www.colgateprofessional.com/Professional/v1/en/us/locale-assets/docs/ACPchairsideGuide.pdf
As always, I appreciate your referrals and am available to discuss any clinical scenarios you may have questions about. I can be reached by phone at 719-576-4247.
Dr. Emily Batson is a native of Colorado Springs, CO. She is a graduate of Indiana University School of Dentistry, and served in the United States Army Dental Corps. She returned to her hometown after completing her specialty training in Prosthodontics at the University of North Carolina at Chapel Hill. She maintains a full-time private practice limited to prosthodontics.
References:
- Bidra A. et al.”Clinical Practice Guidelines for the recall and maintenance of patients with tooth-borne and implant-borne dental restorations.” J Amer Dent Assoc 2016:147 (1): 67-74.