RPDs, or Removable Partial Dentures, are three words when used together generate various facial expressions among dentists, staff, and patients. In the history of American dentistry there is perhaps no greater debate other than occlusion on how and why these prostheses should be utilized. As we have seen advancements with dental materials we have seen extra attention given to flexible partial dentures. This issue of the Byte will examine the materials in use with flexible RPDs, studies behind them, and indications for their use.
- Flexible Partial Denture Materials
Before we look at the materials themselves, let’s remember where we are coming from. RPDs have traditionally been fabricated from two types of materials: Base-metal alloys and acrylics either used in combination or just acrylics alone. Numerous clinicians, including Rudd, Ellison, and Stewart dedicated a large part of their dental careers examining, testing, and implementing “rules” for RPD use. Why do we continue to have such controversy on a topic that many think is a losing battle? The number one reason is because many patients continue to reside on Unhappy Dental Avenue despite use of newer materials to help move them to Successful Dentistry Lane. As with anything in dentistry we have a tendency to try different materials when we have had clinical failures or we want to improve upon a technique. Advancements in lithium disilicates and zirconia appear to be leading us in a good direction for fixed restorations, however we cannot necessarily say the same for removable prosthetic materials.
Flexible partial dentures are fabricated from polyamide denture base resins, or thermoplastic resins. They are commonly referred to as nylon-based partials. Brand names include Valplast and Duraflex. These are not new materials, but have gained momentum over the past ten years by being promoted as “metal-free” partials and more “comfortable” for patients. When searching for clinical research on polyamide denture bases there is not much to review. Most publications deal with bench-top studies examining physical properties that do not necessarily relate to clinical use. There are few clinical studies and case reports, and virtually none with any kind of medium or long-term data. Ito et al1 shared a case report using a nylon-based material to replace a clasp for a Kennedy Class II RPD. At two years the RPD showed favorable results for that particular patient.
Let’s review a couple of details that are of the utmost importance when dealing with RPDs in general:
- Partially edentulous classification
While Europeans were developing sophisticated articulators during the first half of the 20th century, several American dentists worked diligently on classification systems for partial edentulism. Kennedy’s remains the most popular and for good reason. It is simple to remember and apply. We all dread the bilateral distal extension, or Class I scenarios. Next is the Kennedy Class II patient. Lack of distal support can be challenging to manage, and most of these patients have a vertical dimension component to add to your headache. Class III and IV come with different challenges, but having teeth in the posterior segments greatly simplifies your RPD construction for the most part.
The question then arises. Does a flexible, nylon based material solve any problems for these individuals? Partial dentures move as is, so logically it doesn’t make sense that a more mobile, flexible material would help. In reality, nylon based materials are the least desirable materials to use for Class I and II scenarios for the following documented reasons:
- Relines and repairs cannot be accomplished predictably
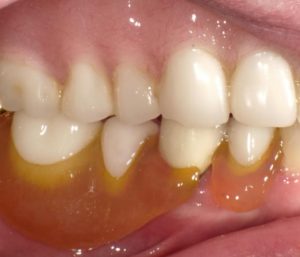
- Color instability (see photo)
- Rest seats cannot be fabricated
- Rigidity of the material suffers over time
Fig 1. Color instability of nylon-based RPD vs. Complete Denture
- The patient you are treating and the remaining anatomy
This is perhaps the most crucial aspect clinicians need to be aware of before stepping into the RPD boxing ring. A patient with xerostomia, limitations with hand mobility, or overall intolerance of removable prostheses will likely not benefit from you surveying and border molding to your heart’s content. Every dental clinician must learn to accept that removable prostheses are not for everyone, despite what Medicaid and dental insurance companies tell you. Furthermore, for the patient who is RPD tolerant, surveying the remaining existing anatomy is crucial. Is there any sort of posterior ridge? Does the patient have a large and uncoordinated tongue? Can the patient allow you to find centric relation repeatedly? Finding the answers to these questions and many others during your treatment planning will help you determine if you can predictably help your patient.
When to Use Flexible Partials
Here are a few indications for use of nylon-based materials.
- As interim therapy
If patients are made aware of the limitations with the material and are in transition to something fixed, flexible partials can be utilized.
- Clasp assemblies for anterior regions
Clasps in the anterior and premolar regions can be substituted with nylon-based clasps, however, longevity may suffer as they distort and discolor over time.
- Small Kennedy Class III scenarios
Nylon based partials can be used to replace a few missing posterior teeth where there are solid adjacent teeth to help retain the partial. Even in these scenarios it is important to be selective when using nylon- based materials.
I hope this issue of the Byte has answered questions you might have regarding flexible RPDs. Although it is important for us to remain flexible in most aspects in life, you should stand rigid in your choice of materials for removable partial dentures. As always, I welcome and appreciate your referrals and am available for consultation by phone or email.
Ito M et al. The combination of a nylon and traditional partial removable dental prosthesis for improved esthetics: A clinical report. J Prosthet Dent 2013; 109.
